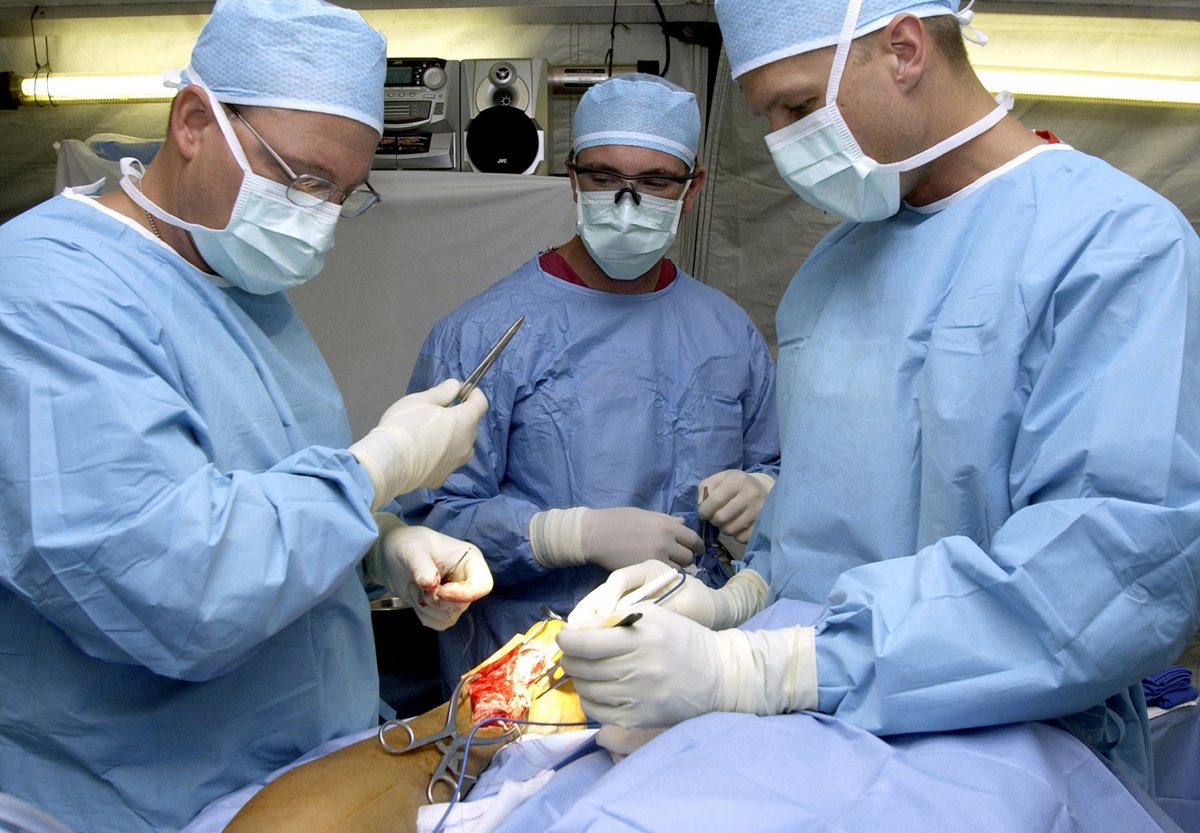
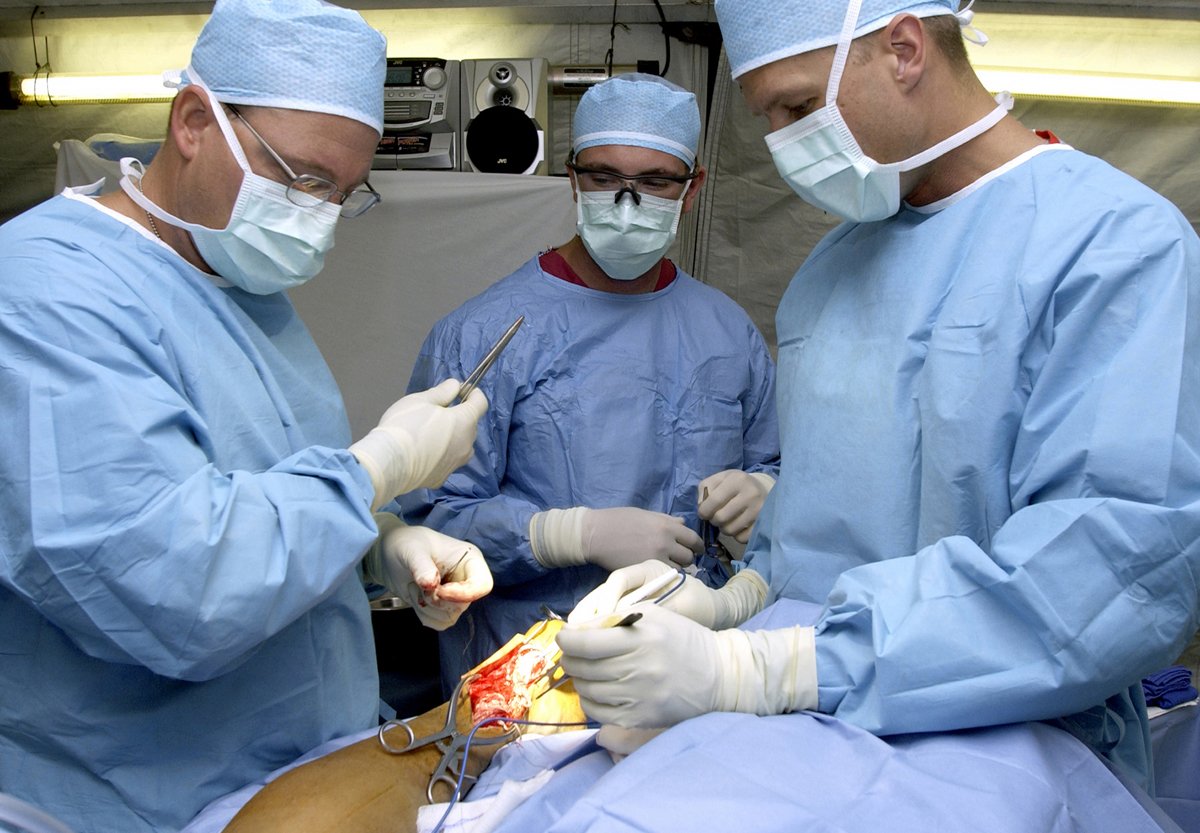
Judith Martin: Should elderly patients risk surgery?
“What older patients want to know is, ‘What’s my life going to look like?’ But we haven’t been able to answer with data of this quality before.”
— Zara Cooper, M.D., professor of surgery at Harvard Medical School and the director of the Center for Geriatric Surgery at Brigham and Women’s Hospital.
Nearly 1 in 7 older adults die within a year of undergoing major surgery, according to an important new study that sheds much-needed light on the risks seniors face when having invasive procedures.
Especially vulnerable are older patients with probable dementia (33% die within a year) and frailty (28%), as well as those having emergency surgeries (22%). Advanced age also amplifies risk: Patients who were 90 or older were six times as likely to die than those ages 65 to 69.
The study in JAMA Surgery, published by researchers at the Yale School of Medicine, addresses a notable gap in research: Though patients 65 and older undergo nearly 40% of all surgeries in the U.S., detailed national data about the outcomes of these procedures has been largely missing.
“As a field, we’ve been really remiss in not understanding long-term surgical outcomes for older adults,” said Dr. Zara Cooper, a professor of surgery at Harvard Medical School and the director of the Center for Geriatric Surgery at Brigham and Women’s Hospital in Boston.
Of particular importance is information about how many seniors die, develop disabilities, can no longer live independently, or have a significantly worsened quality of life after major surgery.
In the new study, Dr. Thomas Gill and Yale colleagues examined claims data from traditional Medicare and survey data from the National Health and Aging Trends study spanning 2011 to 2017. (Data from private Medicare Advantage plans was not available at that time but will be included in future studies.)
Invasive procedures that take place in operating rooms with patients under general anesthesia were counted as major surgeries. Examples include procedures to replace broken hips, improve blood flow in the heart, excise cancer from the colon, remove gallbladders, fix leaky heart valves, and repair hernias, among many more.
Older adults tend to experience more problems after surgery if they have chronic conditions such as heart or kidney disease; if they are already weak or have difficulty moving around; if their ability to care for themselves is compromised; and if they have cognitive problems, noted Gill, a professor of medicine, epidemiology, and investigative medicine at Yale.
Two years ago, Gill’s team conducted research that showed 1 in 3 older adults had not returned to their baseline level of functioning six months after major surgery. Most likely to recover were seniors who had elective surgeries for which they could prepare in advance.
In another study, published last year in the Annals of Surgery, his team found that about 1 million major surgeries occur in individuals 65 and older each year, including a significant number near the end of life. Remarkably, data documenting the extent of surgery in the older population has been lacking until now.
“This opens up all kinds of questions: Were these surgeries done for a good reason? How is appropriate surgery defined? Were the decisions to perform surgery made after eliciting the patient’s priorities and determining whether surgery would achieve them?” said Dr. Clifford Ko, a professor of surgery at the University of California at Los Angeles School of Medicine and director of the Division of Research and Optimal Patient Care at the American College of Surgeons.
As an example of this kind of decision-making, Ko described a patient who, at 93, learned he had early-stage colon cancer on top of preexisting liver, heart and lung disease. After an in-depth discussion and being told that the risk of poor results was high, the patient decided against invasive treatment.
“He decided he would rather take the risk of a slow-growing cancer than deal with a major operation and the risk of complications,” Ko said.
Still, most patients choose surgery. Dr. Marcia Russell, a staff surgeon at the Veterans Affairs Greater Los Angeles Healthcare System, described a 90-year-old patient who recently learned he had colon cancer during a prolonged hospital stay for pneumonia. “We talked with him about surgery, and his goals are to live as long as possible,” said Russell. To help prepare the patient, now recovering at home, for future surgery, she recommended he undertake physical therapy and eat more high-protein foods, measures that should help him get stronger.
“He may need six to eight weeks to get ready for surgery, but he’s motivated to improve,” Russell said.
The choices that older Americans make about undergoing major surgery will have broad societal implications. As the 65-plus population expands, “covering surgery is going to be fiscally challenging for Medicare,” noted Dr. Robert Becher, an assistant professor of surgery at Yale and a research collaborator with Gill. Just over half of Medicare spending is devoted to inpatient and outpatient surgical care, according to a 2020 analysis.
What’s more, “nearly every surgical subspecialty is going to experience workforce shortages in the coming years,” Becher said, noting that in 2033, there will be nearly 30,000 fewer surgeons than needed to meet expected demand.
These trends make efforts to improve surgical outcomes for older adults even more critical. Yet progress has been slow. The American College of Surgeons launched a major quality improvement program in July 2019, eight months before the covid-19 pandemic hit. It requires hospitals to meet 30 standards to achieve recognized expertise in geriatric surgery. So far, fewer than 100 of the thousands of hospitals eligible are participating.
One of the most advanced systems in the country, the Center for Geriatric Surgery at Brigham and Women’s Hospital illustrates what’s possible. There, older adults who are candidates for surgery are screened for frailty. Those judged to be frail consult with a geriatrician, undergo a thorough geriatric assessment, and meet with a nurse who will help coordinate care after discharge.
Also initiated are “geriatric-friendly” orders for post-surgery hospital care. This includes assessing older patients three times a day for delirium (an acute change in mental status that often afflicts older hospital patients), getting patients moving as soon as possible, and using non-narcotic pain relievers. “The goal is to minimize the harms of hospitalization,” said Cooper, who directs the effort.
She told me about a recent patient, whom she described as a “social woman in her early 80s who was still wearing skinny jeans and going to cocktail parties.” This woman came to the emergency room with acute diverticulitis and delirium; a geriatrician was called in before surgery to help manage her medications and sleep-wake cycle, and recommend non-pharmaceutical interventions.
With the help of family members who visited this patient in the hospital and have remained involved in her care, “she’s doing great,” Cooper said. “It’s the kind of outcome we work very hard to achieve.”
Judith Graham is a Kaiser Health News reporter.
Judith Graham: How to talk to seniors, families before surgery
— Photo by I Craig
The decision seemed straightforward. Bob McHenry’s heart was failing, and doctors recommended two high-risk surgeries to restore blood flow. Without the procedures, McHenry, 82, would die.
The surgeon at a Boston teaching hospital ticked off the possible complications. Karen McHenry, the patient’s daughter, remembers feeling there was no choice but to say “go ahead.”
It’s a scene she’s replayed in her mind hundreds of times since, with regret.
On the operating table, Bob McHenry had a stroke. For several days, he was comatose. When he awoke, he couldn’t swallow or speak and had significant cognitive impairment. Vascular dementia and further physical decline followed until the elderly man’s death five years later.
Before her father’s October 2012 surgery, “there was not any broad discussion of what his life might look like if things didn’t go well,” said Karen McHenry, 49, who writes a blog about caring for older parents. “We couldn’t even imagine what ended up happening.”
It’s a common complaint: Surgeons don’t help older adults and their families understand the impact of surgery in terms people can understand, even though older patients face a higher risk of complications after surgery. Nor do they routinely engage in “shared decision-making,” which involves finding out what’s most important to patients and discussing surgery’s potential effect on their lives before setting a course for treatment.
Older patients, it turns out, often have different priorities than younger ones. More than longevity, in many cases, they value their ability to live independently and spend quality time with loved ones, according to Dr. Clifford Ko, professor of surgery at UCLA’s David Geffen School of Medicine.
Now new standards meant to improve surgical care for older adults have been endorsed by the American College of Surgeons. All older patients should have the opportunity to discuss their health goals and goals for the procedure, as well as their expectations for their recovery and their quality of life after surgery, according to the standards.
Surgeons should review their advance directives — instructions for the care they want in the event of a life-threatening medical crisis — or offer patients without these documents the chance to complete them. Surrogate decision-makers authorized to act on a patient’s behalf should be named in the medical record.
If a stay in intensive care is expected after surgery, that should be made clear, along with the patient’s instructions on interventions such as feeding tubes, dialysis, blood transfusions, cardiopulmonary resuscitation and mechanical ventilation.
This is far cry from how “informed consent” usually works. Generally, surgeons explain to an older patient the physical problem, how surgery is meant to correct it and what complications are possible, backed by references to scientific studies.
“What we don’t ask is: What does living well mean to you? What do you hope to be able to do in the next year? And what should I know about you to provide good care?” said Dr. Ronnie Rosenthal, a professor of surgery and geriatrics at Yale School of Medicine and co-leader of the Coalition for Quality in Geriatric Surgery Project.
Bob and Marjorie McHenry pose with their daughter Karen McHenry at their 50th anniversary party in 2009. Bob McHenry had a stroke during an operation in 2012 and was comatose for several days after the procedure. When Marjorie fell and broke five ribs in fall 2017, she decided against surgery after consulting with the hospital’s palliative care team.
Rosenthal tells of an 82-year-old patient with early-stage rectal cancer. The man had suffered a stroke 18 months earlier and had difficulty walking and swallowing. He lived with his wife, who had congestive heart failure, and had been hospitalized with pneumonia three times since his stroke.
Rosenthal explained to the man that if she operated to remove the cancer, he might land in the ICU with a breathing machine and then end up at a rehabilitation facility.
“No, I don’t want that; I want to be home with my wife,” Rosenthal recalled his saying.
The man declined the surgery. His wife died 18 months later, and he lived another six months before he had a fatal stroke.
Surgeons can help guide discussions that require complex decision-making by asking five questions, according to Dr. Zara Cooper, associate professor of surgery at Harvard Medical School:
How does your health affect your day-to-day life? When you think about your health, what’s most important to you? What are you expecting to gain from this operation? What health conditions or treatments worry you most? And what abilities are so critical to you that you can’t imagine living without them?
Cooper recalls an 88-year-old man seriously injured in a car crash arriving in the emergency room several years ago.
“When we started explaining to his family what his life would be like — that he would be highly functionally dependent and not able to live independently again — his wife said that would be absolutely devastating, especially if he couldn’t ski,” Cooper said. “We didn’t even anticipate this was in the realm of what someone this age would want to do.”
The family decided not to pursue treatment, and the patient died.
Sometimes surgeons make the misguided assumption that older patients want to follow recommendations rather than having input into medical decisions, said Dr. Clarence Braddock, professor of medicine at UCLA. In focus groups, 97% of seniors said “I prefer that my doctor offer me choices and ask my opinion,” according to research Braddock published in 2012.
Yet in another study involving older adults, Braddock found that orthopedic surgeons rarely discussed the patient’s role in decision-making (only 15% of the time) or assessed the patient’s understanding of what surgery would entail (12% of the time).
At the University of Wisconsin-Madison, Dr. Margaret Schwarze, an associate professor of vascular surgery, has developed a tool called “best case/worst case” to help surgeons communicate more effectively with older patients.
“The idea is to tell the patient a story in terms they can understand,” Schwarze said.
Instead of citing statistics on the risk of pneumonia or infection, for instance, a surgeon would explain what might happen if things went well or badly. Would the patient be in pain? Would she need nursing care? Would he be able to return home and do things he liked to do? Would she land in the ICU? Would he be able to walk on his own?
A similar range of possibilities is presented for a treatment alternative. Then the surgeon identifies the most likely outcomes for surgery and the alternative, based on the patient’s circumstances.
“Going through a major operation when you’re older is going to change your life,” Schwarze said. “Our goal is to help older patients imagine what these changes might look like.”
Because of her father’s experience, Karen McHenry was cautious when her mother, Marjorie McHenry, fell and broke five ribs in fall 2017. At the hospital, doctors diagnosed significant internal bleeding and a collapsed lung and recommended a complicated lung surgery.
“This time around, I knew what questions to ask, but it was still hard to get a helpful response from the surgeons,” Karen said. “I have a vivid memory of the doctor saying, ‘Well, I’m an awesome surgeon.’ And I thought to myself, ‘I’m sure you are, but my mom is 88 years old and frail. And I don’t see how this is going to end well.’”
After consulting with the hospital’s palliative care team and a heart-to-heart talk with her daughter, Marjorie McHenry decided against the surgery. Nearly three years later, she’s mentally sharp, gets around with a walker and engages in lots of activities at her nursing home.
“We took the risk that Mom might have a shorter life but a higher quality of life without surgery,” Karen said. “And we kind of won that gamble after having lost it with my dad.”
Judith Graham is a Kaiser Health News reporter.
Judith Graham: khn.navigatingaging@gmail.com, @judith_graham